Category: Family Stories
Learning to Breathe
Published by Athena Flicek on Apr 10, 2024
I could feel my blood pressure rising. You might wonder if I was about to run a race or perform a medical miracle. All I was doing was sitting at the dining table for lunch with my 4-year-old son. Looking at his sweet face. My eyes staring back at me. All of a sudden, I couldn’t breathe. He had bitten off a large piece of chicken. I was waiting for him to struggle to manage it. It sent me into a familiar spiral, presenting me an image I had been confronted with since he was an infant. Him struggling in front of my very eyes. He did amazing, as usual. And in that moment I realized that I needed help.
No one had told me I needed help up to this point. They could see it but they remained silent. They saw me struggle to leave my bedroom or to wash my hair. I would tell them I hadn’t brushed my teeth in over a week, and honestly, if you know me (a child who had braces, an expander, a retainer, and lover of floss and white strips) this would be the most obvious scream for help. Yet nothing. Nobody knew what to say or what to do.
But today was different. Today I could feel my anxiety clawing to get ahold of my child. And I knew I had to get help. I was 39 when I searched for support. It took me a year to build up the courage to schedule an appointment. It was my 40th birthday present to myself. Speaking of birthday’s, let’s get back to a very important one: my son Ari’s.
I had a beautiful pregnancy. Then came the struggle. Over the first 48 hours I heard him constantly struggle to clear his amniotic fluid. I would freeze up. His dad would grab the suction and get it out. When they told us we could go home I had a gut feeling that something wasn’t right. I felt like my son needed more testing or help.. I didn’t know what, but something felt off.
Over the next 18 months Ari would projective vomit across the room after every meal. He couldn’t sleep laying down. Every visit to his pediatrician’s office ended in tears. “It’s just spit up,” they said. Well, I knew that wasn’t true. My child’s body was violently refusing milk and certain foods. But here I was, trying to airplane an unwanted food into his mouth. At the end of one visit my son’s doctor casually said “You might want to try this local nonprofit, they might have some resources to help.”
I hurried home, went to their website, and all I could see was their beautiful orange “Get Help” button. I clicked on it seemingly 300 times. They had a simple 6 item feeding questionnaire to complete and be able to tell if your child might need help. If you answered affirmatively to 2 of the 6 it directs you to help. I answered affirmatively to all 6 and immediately started crying. My son Ari has pediatric feeding disorder. You might wonder what that is. It’s a child who isn’t eating in an age-appropriate manner. Ari also has EoE (eosinophilic esophagitis) and sensory processing disorder (PFD). He is curious, fast, a born performer, comically inclined and wants to build robots that he can accompany to space one day. I quit my job as an elementary school teacher to take him to therapy and help him find joy in food instead of fear.
It was the beginning of the end for many things for me: my marriage, my first career. But it was also the beginning of a new and amazing experiences.
Ironically, right before I started therapy, I saw a job posting from the same non-profit that I felt had saved me and my son. It was for someone to plan their annual pediatric feeding disorder educational conference. I didn’t tell anyone about it. And then I made it to the third round. I will never forget that phone call and subsequent job offer. They gave me a gift. A gift I will never be able to repay. Planning a pediatric feeding disorder conference for families and professionals is part of my therapy.
I feel like we are all given gifts. Ari was another one. He has taught me that his journey is not mine. I’m just a guide. My anxieties, should not be his. And my therapist likes to remind me I’m not a doctor, a mind reader or a fortune teller. I need those daily reminders. Therapy has taught me to avoid negative thoughts, be independent instead of co-dependent (and yes, this includes how we interact with our children), and to live in my calm, peaceful place.
I finally took my first deep breath two months ago. I could tell it was different. I am not a failure because I couldn’t feed my child. I am a success because of it.
PFD Story- Baking with the Besties
Published by Christina Van Ditto on Mar 28, 2024
As parents of children with medical complexities and special needs, we parent as clinicians. We are responsible for care and carryover that often resembles a therapeutic and medical model.

When Gia was a toddler, I ran our home like one big therapy session. About six months into it, she was miserable and so was I. This approach wasn’t working for either of us. So, I ditched it and committed to simply being Gia’s mom. I leaned into what feels natural to me, a method I refer to as, “instinctual parenting”.
When it came to language and regulation, as a former dancer, I used movement and dance to encourage verbalization, soothe, and bond with my daughter.
And when Gia didn’t respond to intensive therapies for ARFID and she began her journey of being tube fed, I leaned into what felt natural to me once more.
I put on a show. Literally.
A supportive baking show
Welcome to Baking with the Besties, where fashion meets inclusive baking. A baking show that I have been putting on for my daughter for several years now.
The planning process is nothing short of involved.
Each month’s theme is carefully considered. In addition, there’s the recipe which needs to be gluten and dairy free and relevant to the theme. I consider the sensory profile of each ingredient that we’re using and handling. Sensory supports that are always accessible to Gia are a bowl of warm water and dry towel when she needs relief from a tactile sensation and headphones for the times we use the mixer.

And there’s the fashion, which is not superficial.
Again, this approach is instinctual to me. To me, fashion is a form of self-expression and I am incredibly passionate about accessible and adaptive fashion, subsequently. Imagine my surprise when Gia, 4 years old at the time, refused to change out of a Frozen t-shirt for three months. I even had to bathe her in it. Through this experience, I learned that Gia’s insistence on sameness was her go-to, functional way to manage her anxiety.
Therefore, I use fashion as a tool to encourage cognitive flexibility in Gia, I call this “Flexibility through fashion”. She is able to transition in and out of outfits and costumes that we wear with joy, excitement, and interest. In addition, I design and create custom chef hats. Nowadays, we have more of these glamorous and over the top chef hats than I can count. I’m always surprised as to how beautiful they come out and just cannot wait to show Gia the finished product that I make specifically for her. It doesn’t end there. Sometimes the monthly theme calls for us to wear wigs. Which challenges her sensory assimilation in a super fun, non-threatening way.
Bringing awareness and acceptance
When it comes to exploring the food that we’re handling, Gia is never expected or pressured to eat what we make. Nearly two years in, during our first few episodes Gia was repulsed by the smell of flour. Her olfactory is super sensitive and at that time, was working overtime as her body was healing from nutritional deficiencies.

When disinterest sets in, it isn’t uncommon for me to use Gia’s special interests to encourage her to interact and engage. Small figurines, lined up in batter, make regular appearances in our episodes.
We research and learn the person or the topic that we’re celebrating with food that month. Most importantly, we celebrate one another. And enjoy the messes we make along the way. There’s laughing, crying, and stimming. We bring awareness to feeding differences and acceptance to neurological differences.
Our therapy room is our kitchen and the work is done at our baking benches. Gia has her own drawers filled with her own cook books, measuring cups and plastic safe cutlery. Another strategy and invitation for a person that has never used cutlery to eat … she’s 8 years old. We have cake stands that spin, she’s a big fan of that. As a visual learner and hyperlexic, Gia loves and thrives with visuals, so we love a good recipe in print. And the cook book stand often doubles as a holder for her transitional book.
Supporting Gia

Gia has one safe food. And one safe beverage. Brand specific and presented in only a few variations, with a ritual. Gia moved from an NG to a more long term solution to meet her nutritional needs of a Mic-key button.
There’s no shame in our game. I’m just a mom baking with her daughter. Who happens to be neurodivergent and tube fed.
Gia is learning that food is more than what we put in our mouths. It brings people together, oftentimes the people we love most. We are building happy memories and learning food is a gift to give. Food represents mealtimes where everyone has a place at the table, regardless of what’s on or not on our plates. Essentially, she is building positive neuro associations with food and eating.
BWTB’s truly is more than a baking show we record from the comfort of our ASD friendly kitchen. Oftentimes laughing before we even hit the record button, It has helped to reduce the stress and pressure around eating and mealtime for us both. A natural modality, I have used my creativity to support Gia in her recovery and help to alleviate caregiver stress, simultaneously.
A journey beyond the kitchen
A part of my journey as a caregiver and food partner to my daughter has been letting go of expectations and standards. Eating and pediatric feeding disorders, different abilities, and medical complexities can be disempowering. I am not minimizing the worry or overwhelm that we justifiably experience as parents and caregivers. Gia has never put a morsel of meat in her mouth. She would be unable to safely masticate a chip or fibrous, non-pureed fruit or vegetable, at this time. But Gia is on her own time-line. And I am finally at peace with that. I felt so much urgency at the start of our journey. A familiar pang I felt in regard to her developing language and learning to toilet. Now, I understand and have embraced that we are not in race. My child is building new pathways, developing and strengthening her sensory muscles, working through debilitating anxiety and cognitive flexibility. And the whole while, I never take off my mom hat. Or my mom chef hat, that is.
Recovery is a journey. And I’m here for it. I am more than my daughter’s food partner, I am her partner in life.
This is Gia’s journey with food, only it’s more of a screenplay than a story and the last Act has yet to be written.
Stay tuned.
Christina Van Ditto is a PFD and ARFID caregiver, advocate, writer and public speaker.
Insider insights: Preparing for your child’s G-tube journey
Published by Feeding Matters on Feb 26, 2024
What to expect before and after your child’s G-tube insertion
So, you’ve finally decided to get a G-tube for your child. Arriving at this point in your child’s feeding journey can be a relief. Others may feel some regret.
Either way, says Karen Ellis, mother of a 2.5-year-old who recently got a G-tube, getting a G-tube can make life a lot easier for children with pediatric feeding disorder (PFD) and their parents. After a minor procedure, a short recovery and months of stress-free feedings, Ellis and her family are confident they made the right decision for their son.
G-tube insertion, or gastrostomy tube insertion, is a medical procedure where a tube is placed through the abdominal wall and into the stomach. This allows caregivers to deliver nutrition and medications directly into a child’s stomach. Some kids with a G-tube use it to supplement oral feeding. Others exclusively eat and drink through the device.
Learn more about the benefits for kids with PFD of G-tubes in this blog: Does your child need a G-tube? Here’s what you need to know.
Ellis’s son, Ishan, gets most of his nutrition through the G-tube. He eats and drinks orally as well. Ellis offers insight into what parents can expect from the G-tube procedure and the few months after it.
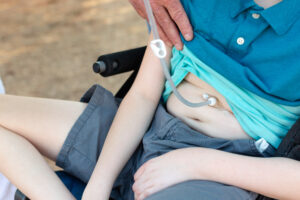
What to expect before the G-tube procedure
Ishan had an NG tube for a longer period than typical, says Ellis. Running after an active toddler to replace the tube whenever it fell out was a constant struggle. Since birth, Ishan has struggled with eating due to gastrointestinal issues and silently aspirating. He was often sick, didn’t eat age-appropriate amounts and was slow to gain weight. His parents pushed Ishan’s providers to consider a G-tube, but they were told their son might grow out of his feeding issues.
At this stage of the PFD journey, Ellis says following your instinct as a parent is essential to advocating for your child’s needs. “They wanted to blow everything off as normal parenting or a simple therapy issue, but knowing as a parent that there continues to be something wrong means you have to keep pushing,” she says.
What gave Ellis clarity, she says, was knowing they were trying hard enough. “He was doing his best, we were doing our best, but still, something was not quite right.”
What to expect during the G-tube procedure and recovery
For Ellis, the hardest part of the G-tube procedure was knowing it was elective surgery that required hospitalization. By the time Ishan was scheduled for surgery, Ellis knew it was necessary, but she still felt they had made a choice. Ishan’s procedure and recovery both went smoothly.
Like most kids, Ishan spent one night in the hospital. Ellis says he did experience some pain that first and second day. Ishan received pain medication and lots of TLC. They held him the whole time at the hospital and watched his favorite programs.
By day three and four, Ishan was back to running around and doing his typical gymnastics flips. He returned to his normal toddler antics in less than a week. “Kids are resilient, but we tried to hold him back from too much activity right after surgery,” she says.
For two weeks, Ishan had to skip his baths and only have sponge baths. In general, swimming in the pool or ocean tends to be okay, but lakes and rivers can be problematic.
Watch the skin around the G-tube because that can start to look angry and red initially. You can learn more about feeding tube care using What You Need to Know Now: A Parent’s Introduction to Tube Feeding. This resource, also provided in Spanish, was provided by the Feeding Tube Awareness Foundation with permissions to share.
What to expect in the months after a G-tube procedure

Adjusting to G-tube feedings takes some trial and error for parents and kids. Even months later, G-tube feeding requires adjustments when a child is less hungry due to an illness or more hungry due to a growth spurt. In the beginning, says Ellis, it’s important to go low and go slow with feeds.
At first, Ishan hesitated to let anyone touch his stomach, so his parents made buttons for his favorite stuffed animals. They fashioned these themselves, but you can also buy them. Ellis showed Ishan how opening and closing the button doesn’t hurt. They spent a lot of time talking about the button and getting used to it before diving into feeding.
Ellis also spent some time getting used to feeding her son through the tube. Overfeeding can cause vomiting or an upset stomach. She keeps a towel in the car in case of any incidents. “It’s hard to guess how much a toddler wants to eat. It’s never a perfect science,” she says.
Ellis offers three tips for G-tube feeding
- Find the formula your child tolerates best. Like baby formula, G-tube formulas come with different ingredients. The Ellis family found that the vegan formula has been better for Ishan than the milk formula.
- Stay consistent with oral feeding when applicable. Ishan eats orally two times a day. They do this before tube feeding so that his stomach isn’t full.
- Use a backpack. Cute feeding backpacks allow busy toddlers to run around independently during feeding sessions. Ellis tapes the tubing to the back of Ishan’s shirt or pants so it doesn’t come out while he’s running around.
These days, Ishan is happily playing and growing, and his parents are confident they made the right decision to get a G-tube. Ellis says it’s helpful to consider the G-tube feeding experience with PFD more like a marathon than a sprint. This can be harder for parents than kids, who tend to be more resilient. “As long as the kid is pretty happy and healthy, we’re the ones who are more stressed,” she says.
For more support in your G-tube or pediatric feeding disorder journey, check out our peer-to-peer mentoring program.
A story of triumph over pediatric feeding disorder
Published by Feeding Matters on Feb 15, 2024
The way pediatric feeding disorder (PFD) manifests in each child is as varied as the children themselves. But so many stories of parenting children with PFD are the same.
An infant struggles to feed and gain weight. Parents work tirelessly to feed their children and juggle medical visits. They search in the dark for a diagnosis of a complex problem they don’t understand, all while feeling alone and at fault.
Raising a child with PFD is a journey that rarely has a final destination. With the right support and care, it does get easier. This is the story of one mom of a son with PFD and how she’s gone from seeking help to supporting others.
One family’s journey with PFD

From the start, Erin Avilez’s son, Julian, struggled to breastfeed and gain weight. Her doctors were concerned about her baby’s measurements throughout her pregnancy. When her amniotic sac fluid was low, Avilez was induced at 37 weeks.
Julian was born at 5 pounds and right away had trouble sucking and taking in enough food at each feeding. Avilez switched to bottles, but Julian continued to undereat. “Within the first few months, there were already red flags that he was underweight and not getting enough nutrition,” she says.
Avilez and her husband started by switching formulas to see if Julian had some sensitivity to some ingredients. Still, they didn’t see much weight increase. Things got worse when her pediatrician sent Julian to a pediatric gastroenterologist. “That’s kind of where the horror of the story started,” she says.
Julian’s pediatrician and the GI weren’t communicating or working together and sometimes had different goals. “The GI’s only goal was for Julian to gain weight and cared less about how it affected his feeding,” says Avilez.
Julian got a nasogastric tube (NG tube) at three months old. The increase in calories made him vomit a lot, and he regularly pulled the tube out. Any time he pulled the tube out, Avilez would have to call her husband to come home from work so the two of them could force the tube back in. Insurance only covered a few tubes, making this devastating ritual even more difficult. Julian developed an oral aversion that he never had before and wouldn’t even let his parents touch his face. By seven months, Avilez insisted the NG tube be removed.
When Julian’s GI recommended a gastrostomy feeding tube (G-tube) instead, Avilez knew they needed a second opinion. Julian took some formula and solid foods orally, and Avilez thought they could build on that. A new GI at Phoenix Children’s Hospital agreed.
With a new pediatrician and GI, Julian’s doctors started working on finding a diagnosis. He was also able to join their intensive feeding therapy program. “The new GI doctor we saw listened, and he offered empathy and support,” says Avilez.
When Julian was 3.5, his family finally got a diagnosis of what caused his pediatric feeding disorder. A liquid and a food study showed that he has gastroparesis, a condition where the stomach muscles do not work properly to empty waste.
Now that Julian has a diagnosis, he’s able to take medication to help his gastric delayed emptying, as well as an appetite stimulant. He also drinks Ensure Clear to add more calories to his diet. Julian has an aversion to any formula or dairy because of his early experience with the NG tube.
In the past six months, Julian was finally registered low on the weight chart for the first time. “This is huge for him,” says Avilez.
Still, says Avilez, their struggle is never far from her mind. She dreads visits to the pediatrician when she knows Julian will be weighed. “Even today, a week before his appointments, I start getting stressed out because I know we have to get on the scale,” she says.
Finding support from other families with PFD
Julian was born during the pandemic, and Avilez left her job as a social worker to take care of him and to get to all his appointments. She suffered from postpartum depression and felt overwhelmed, alone and isolated.
“I knew there has to be some type of service out there to help moms like me,” she says.

Avilez searched online and found Feeding Matters. She requested a peer-to-peer mentor and was matched with another mom who shared her experience. That empathy was powerful. “She listened to me. The first time I got off the phone with her, I started crying that somebody understood what I was going through,” says Avilez.
Avilez’s mentor also told her she was doing a great job. “Throughout this process, nobody told me I was doing a good job, not the doctors or anyone on his care team,” she says.
Avilez’s introduction to Feeding Matters was the first time she learned about PFD. “I felt so validated that we weren’t the only ones concerned about not knowing what was going on with our son and not hearing about it from our doctor,” she says.
Today, Avilez is a peer mentor to other parents raising a child with PFD. She’s grateful to have support and to be able to pay it forward. Her hope is that more clinicians and hospitals will inform parents about PFD from the start. “I wish that when you have a child with feeding difficulties, someone from the start would offer resources,” she says.
Key takeaways for supporting your child with PFD
Avilez offers the following advice to parents raising a child with PFD.
- Find a supportive care team: If the doctor’s not listening, find a more supportive provider. Having a good team in place makes all the difference.
- Trust your instincts: It’s okay to get a second opinion and ask questions. Keep advocating for your child because you know your child best.
- Find friends, family or a peer mentor: Find someone who will listen and understand so that you feel less alone.
Behind the headlines: Exploring the complex world of tongue tie releases and pediatric feeding disorder
Published by Feeding Matters on Jan 29, 2024
A tongue tie release procedure (frenectomy or frenotomy) is increasingly prevalent among children with pediatric feeding disorder (PFD) that the majority of them have had it, or their parents at least considered it.
That’s because difficulty breastfeeding is common among children with PFD. A frenectomy is often considered an early treatment to improve latching while breastfeeding.
Breastfeeding is a complicated process that doesn’t come naturally to all mothers and babies. It takes multiple muscles, the ability to coordinate sucking and breathing and the strength to stay awake through strenuous exercise. Releasing a tongue tie can seem like an easy fix.
But for kids with PFD, a frenectomy doesn’t necessarily fix feeding problems and is instead one step along a journey of treatment when the frenulum is not the sole cause for feeding dysfunction. For some babies, a frenectomy can be helpful. For others, it’s not necessary. And in some rare cases, the elective procedure causes harm. While generally safe and often performed by dentists, the procedure maintains the potential to do harm, without a significant assurance of benefit. The procedure is sometimes not covered by insurance and can cost hundreds of dollars.
The debate about releasing tongue ties recently was brought to the forefront in The New York Times article, Inside the Booming Business of Cutting Babies’ Tongues. Showcasing many cases where the procedure was unnecessary or went wrong, the article paints a picture of a procedure as controversial as it is common.
Tongue tie releases for children with pediatric feeding disorder
What’s clear from working with countless families of children with PFD is the benefits of a frenectomy vary on a case-by-case basis. Most importantly, it should never be a result of a self-referral to a clinician who advertises the procedure as the obvious answer for breastfeeding difficulties. Instead, the decision should be shared by the family and a qualified clinician.
Nikhila Raol, MD, MPH, pediatric ENT and an associate professor at Emory University School of Medicine who researches ankyloglossia, or tongue ties, says getting the procedure is a multifactorial decision, meaning it
takes careful consideration with advice from multiple clinicians working together. “Even when the tongue tie is physically obvious, I’m still a proponent of having a functional evaluation with a feeding therapist or lactation consultant with real expertise in evaluating feeding and latch before a procedure. What I’m finding in my ongoing research is that even if a baby has a tongue tie, if the mother’s breast shape is favorable, it may not cause as much issue as we think,” she says.
Breastfeeding often takes some time for babies and moms to adjust. Dr. Raol recommends most parents wait at least two weeks to a month of trying ways to adjust to breastfeeding before getting a frenectomy on a newborn, assuming that the weight gain is acceptable. “Sometimes, you just have to give the baby time to figure it out and the mom’s body to adjust to breastfeeding. Figuring out how to latch and how to get a strong suck sometimes just get better with time,” she says.
Jaclyn Pederson, CEO of Feeding Matters, sees many parents consider the benefits of a frenectomy when breastfeeding or picky eating is challenging. As a parent, she did the same and released the tongue tie on one of her sons. She says that while a tethered tongue is a concern, what can get lost is the nuance that it’s one concern of many –– especially when a child is diagnosed with PFD. “What we know about PFD is that it’s incredibly complex. One of the first things that we share with families is helping them understand that there’s not just going to be a switch that’s flipped to make their feeding journey easier. It’s a series of small milestones that build over time,” she says.
The challenge of considering a frenectomy as a quick fix to difficulty breastfeeding is not just disappointment when it doesn’t work. It can mean overlooking the actual root of the problem, such as some other problem with feeding or swallowing. “Assuming that the surgery is the solution, even as minimal of a procedure as it is, still leaves out a lot of other feeding components,” says Pederson.
One family’s tongue tie release story
When Emily Garlinsky’s son, Landon, had trouble breastfeeding, she was at first confident a tongue tie wasn’t the issue. Clinicians in the hospital when he was born, as well as her pediatrician, assured her his tongue looked normal.
But as Landon continued to struggle and Emily shared her feeding frustration in Facebook groups, she kept hearing people recommend a tongue tie evaluation. By the time Landon was four months old and still struggling to feed, Emily thought it was time to revisit the issue. Landon was already in feeding therapy at that point, and his therapist agreed the procedure might help.
Emily went to a pediatric dentist who told her Landon had a lip tie and a tongue tie. Landon underwent the procedure, but his feeding didn’t improve. He did well with the surgery, though, and Emily is glad they did the release. “There’s a lot of back and forth on Facebook groups from people who regret it. It didn’t help with feeding for us, but other aspects of the release are helpful for speech,” says Emily.
True or false? Tongue tie myths
Dr. Raol warns against peddling fear to encourage parents to act for their babies or overpromising treatment results. “You must be careful because breastfeeding mothers are a vulnerable population. A new mother just wants to do her best,” she says.
Following are some common assumptions around tongue tie release procedures. Some have no research evidence to support them, and others have emerging research.
Tongue ties cause swallowing difficulties: Maybe
Dr. Raol is rigorously studying this in her research. She says, “When you swallow, your tongue starts the pharyngeal squeezing process. When a child can’t squeeze hard, we think this could cause food or liquid to spill into the airway as it is trying to enter the esophagus.”
Tongue ties cause reflux: Unknown
Reflux is normal in babies due to low tone of the sphincter muscle that separates the stomach from the esophagus. Dr. Raol explains that it has never been objectively demonstrated that a tongue tie is responsible for this through aerophagia, or swallowing air, which is the proposed mechanism. However, some studies have shown that reflux symptoms improve after frenectomy. What we do not know is if the symptoms would have just gotten better with time.
Tongue ties cause problems with craniofacial development: Maybe
There’s not a lot of existing research evidence to support this. More research is needed.
A laser is better than clipping for a tongue tie release: Maybe
Many parents hear on social media advice to go to a pediatric dentist instead of an ENT for a tongue tie release because dentists use a laser.
More research is needed, but a review of the existing research found the laser procedure resulted in a shorter surgery, without suturing, and less postoperative pain.
Tongue ties cause speech issues: Maybe for some
The jury is still out on this because Dr. Raol explains there is a deficiency in the literature. Most of the research comes from English-speaking countries, but there’s a difference in how the tongue works in other languages. “In Indian languages, we use the tongue a lot more with certain sounds where you put your tongue far back on the palate. In India, the primary reason kids get a frenectomy is for speech.”
For serious speech issues, though, says Dr. Raol, a tongue tie release is not a quick fix. “In the case of expressive aphasia or something like that, we should not be telling families that clipping a tongue tie will solve that problem,” she says.
You should go to a pediatric dentist for a frenectomy: Only with a diagnosis or consultation from an ENT, lactation consultant, feeding skill specialist, or pediatrician first –– and in that case, the ENT or a pediatric dentist could do the procedure
Breastfeeding is complicated, and any issues should be evaluated by an expert who considers both the baby’s and the mother’s anatomy. Misdiagnosing a tongue tie as the issue can mask other underlying problems, such as PFD.
While it’s true that a frenectomy is a minor surgery and a trained clinician can safely manage the procedure, it still requires careful consideration.
Be wary of a clinician who promises the procedure as a quick fix in exchange for out-of-pocket payment.
Signs your child might need an evaluation from a feeding therapist or lactation consultant
While some children’s tongue ties are apparent even to the untrained eye, it’s still important to get a thorough evaluation before scheduling a frenectomy. Under no scenario should you self-refer or decide based on advice from a friend or a clinician on social media. While this may seem obvious, many people are doing just that and then paying cash for the elective procedure. “We’ve seen this become the number one thing families are thinking about when they have trouble breastfeeding because they hear their friends talk about it and see it online,” says Pederson.
Following are some signs your child might be a good candidate for a frenectomy:
- Your child is not steadily gaining weight from breastfeeding.
- There is some tongue tethering.
- Pain while breastfeeding goes beyond the initial adjustment period.
- You’ve tried various positions and breastfeeding techniques.
- The number of times your child feeds per day remains the same over time. Your baby should become more efficient at feeding as she grows.
When seeking the right clinician, Pederson recommends starting with your pediatrician and an ENT, who will conduct a thorough evaluation. “Look for a professional who shares the pros and cons of a scenario versus one who pushes a treatment as the answer to everything. Explaining the nuance is how you know that a professional really understands how complicated tongue ties are and the issue of feeding is in general,” she says.
Like any treatment or therapy for children with PFD, managing feeding requires a degree of personalized medicine. “Some kids really do need a frenectomy. But if all I have is a hammer, everything is a nail. The tongue is just one piece of the puzzle,” says Dr. Raol.
In the end, getting even a minor tongue tie release surgery is a decision parents should make based on clinical advice, says Dr. Raol. “If you’ve tried everything, and there does seem to be some tethering, and you’re fully aware that this may or may not help, then I don’t think the procedure is unreasonable.”
Feeding Matters blog posts are written by the communications team at Feeding Matters and designed to continue the conversation and awareness around pediatric feeding disorder based on expert opinion interviews.
MY PFD JOURNEY: JAX
Published by Amber Mieras, Family Advisory Council Chair on Feb 14, 2024
Meet Amber and Jax Mieras. Amber is the Pillar Chair for Family Support and is also the devoted mother to nine-year-old Jax, who has Down syndrome. We invite you to join us on their PFD journey and follow their compelling narrative describing the intricacies of Jax’s care. Read Amber’s introspective reflections and see the inspiring results of parent directed care. View Chapter 1 of their story here.
Chapter 2: How to prepare for your child’s evaluation and questions to ask.
While preparing for our evaluation, I reached out to other pediatric feeding disorder (PFD) families and individuals I’ve met through Feeding Matters for advice. I outlined the opportunity to return to treatment and asked, “What should I ask during my evaluation?” I was quite impressed with the feedback I received.
Three major themes emerged from the questions posed: Theme 1: A call for a family-focused approach.What are our family’s aspirations for Jax within this program? Honestly, I struggled with this question initially. Over the years, I’ve relied heavily on the guidance of medical professionals and other families. Our own family had never explicitly discussed what truly mattered to us. We determined that while a reduction in Jax’s gastronomy tube volumes would be great, our paramount goal was for Jax to develop a genuine enjoyment for food and the mealtime experience.
Consequently, one of my primary questions became, how can we help Jax develop a healthy relationship with food, addressing both his physical and psychological needs, as well as those of our family?”
Theme 2: A call for evidence.The next questions centered on evidence based practices. What does the long-term data of patients look like, not just at the time of program discharge, but weeks, months, and even years down the road? How does the program define success and how frequently is this success measured? How is this information communicated to parents?
Theme 3: A call to recognize our child as a unique individual.Finally, the focus shifted to Jax himself — his unique needs, challenges, and complex history with eating.How will you adjust your program if something isn’t working? How will you create a program that maximizes his chances for success? If his behaviors begin to impede his progress, how will you address this challenge? How do we address his relationship with food before focusing on his eating skill and volume?
I entered the evaluation terrified but prepared. I had meticulously recorded my questions in the medical notebook I took with me everywhere. I was blown away with the responses I received from the feeding therapy team.
I expected push back, I thought they might view me as “that mom” or tell me Jax’s case was too complicated. Instead, they acknowledged our journey. They acknowledged our hard work, how far he had come in 5 years, how ready he was for their program. They recognized his maturity, his improved skills, and his willingness to engage more, even if he still didn’t have a love for food. Before I could even start with my questions, they asked me, “What are your goals?” This made it obvious to me that this was going to be a different experience for us. Our team started this new journey by demonstrating their willingness to work with us and by demonstrating their desire to provide the best possible help for Jax.
Rather than making promises of high percentages of success, they showed flexibility and a commitment to reflect on each day and week while involving me as part of the team. They explained what they hoped to accomplish and how goals would be constantly adjusted. The team aimed to meet Jax where he was while challenging him without inducing stress.
I can’t explain the feeling I had leaving that evaluation. I felt empowered. I felt heard. I felt hopeful. These are things I hadn’t felt for a long time when it came to Jax’s feeding challenges. I knew this would be hard, but I also knew in the depths of my soul, that it was the right time and the right program. Jax was ready and so was I. We weren’t expecting miracles, just help and support, and we couldn’t wait to get started!
Find questions to ask providers when seeking treatment for a child with pediatric feeding disorder here.
Follow the next chapter in Amber and Jax’s story by visiting our blog regularly. Updates to come!
My PFD Story: Georgio
Published by Gia Licata & Nicholas Matthews on Dec 19, 2023

We tried for over a year to get pregnant and we couldn’t have been happier when we found out I finally was. After many loses, medications, and tears.. our miracle baby was here. Something wasn’t right though, and I knew that from the minute I found out I was pregnant.
They diagnosed me with Polyhydramnios and told me there was nothing to worry about. Right. After googling for days, I was reading a lot of baby’s having swallowing issues in links to the polyhydraminos. This worried me a lot and I spoke with my doctor and she reassured me that that wouldn’t happen. Georgio was born at 35 weeks and spent 5 days in NICU. As I mama, I knew something just wasn’t right. He was vomiting his feeds, super fussy and something just really seemed off.
On January 5, 2023 Georgio was hospitalized for ten days after he completely stopped eating. A bunch of tests showed that he had dysphagia and was unable to safely eat. By April, he had a G-tube put in and I really believe that’s the day our journey truly began.
Running to the grocery store is no longer a simple task. Routines don’t exist. Date nights aren’t even an option. Snuggling rarely happens. To say our hearts are broken, is an understatement. I sat in that space for months. But then I realized that my 4 month old was now a 10 month old. Time went. I stayed in that space, but time moved forward. That’s when I realized that I had to just come to terms with this being the way it is.
I like to say for now. I like to have hope. I have to say that things have gotten better. My son was on basically a continuous feed all day and now gets 3 feeds each day and 1 overnight. We have gotten his overnight down to 5 1/2 hours and we also even managed to get him feeding safely in his crib.
I worry everyday that my son won’t have a “normal” life, but I try to remember that this is HIS “normal”. He doesn’t know any different. He’s the happiest baby, always laughing. That’s where I find that hope I was talking about. You have to stay hopeful, because at the end of the day they need us.
I remember the days where I would cry because I knew my baby was going to be hospitalized for dehydration because I couldn’t get him to drink. Now, I know he’s eating. He’s healthy. He’s gaining weight. We have to remember that even though things are different, our babies are fighters. They’re strong. They’re resilient.
Georgio is a true miracle. He lights up every room he is in. He truly is the strongest kid I know and will forever be my hero.
My PFD Story: Ashley
Published by Ashley Collier on
 My daughter was a 33-week preemie and hated to be fed. We were discharged from the NICU without reliable feeds and tried to outrun a feeding tube for years. She got one when she was 2 1/2 and made tremendous progress. We also fumbled with some not-so-knowledgeable professionals who should have known better, but we finally found a good feeding team when she was 2.
My daughter was a 33-week preemie and hated to be fed. We were discharged from the NICU without reliable feeds and tried to outrun a feeding tube for years. She got one when she was 2 1/2 and made tremendous progress. We also fumbled with some not-so-knowledgeable professionals who should have known better, but we finally found a good feeding team when she was 2.
After intensive feeding therapy at age 4, we got to wean off the tube and she is now eating typical food in an almost typical way. She has overcome GERD, oral motor issues, slow motility, texture and flavor aversions, and all the learned associations from those.
It’s been quite a journey and as were living it there was nobody to connect with to try to find a better way or just a place to vent. I volunteer now — my daughter is 15 — to help make sure no family after us fumbles the way we had to.
My PFD Journey: Jax
Published by Amber Mieras, Family Advisory Council Chair on Dec 07, 2023
Meet Amber and Jax Mieras. Amber is the Pillar Chair for Family Support and is also the devoted mother to nine-year-old Jax, who has Down syndrome. We invite you to join us on their PFD journey and follow their compelling narrative describing the intricacies of Jax’s care. Read Amber’s introspective reflections and see the inspiring results of parent directed care.
Chapter 1
 I am the proud mother of two kids, Nayeli, 5, and Jax, a 9-year-old boy with Down syndrome and PFD. I found out while I was pregnant that Jax had Down syndrome but had no idea that eating struggles would end up becoming the biggest challenge we would ever face.
I am the proud mother of two kids, Nayeli, 5, and Jax, a 9-year-old boy with Down syndrome and PFD. I found out while I was pregnant that Jax had Down syndrome but had no idea that eating struggles would end up becoming the biggest challenge we would ever face.
Jax had his first diagnosis of failure to thrive at just eight days old, and then again at 4 months of age. After four months of dream feeding, counting milliliters, watching the clock, and witnessing Jax’s struggles, we knew he needed more help to get nutrition. We consented to a nasogastric tube and fourteen months later, Jax got his gastrostomy tube. He could not eat what he needed by mouth alone.
Over the next nine years our family was on a mission. Our goal was not only to help Jax become more comfortable around food and mealtimes but also to better understand the root cause of his oral aversion and PFD. We were determined to find ways to support both him and our family through this challenging journey.
For several years, Jax had weekly feeding therapy at a nearby children’s hospital. We observed periods of progress followed by significant setbacks. Despite the therapists’ dedicated efforts to explore various strategies and approaches, nothing seemed to stick.
When Jax turned 5, we participated in an intensive outpatient feeding program, with little improvement. The following year, at the age of 6, we enrolled in an intensive inpatient feeding program, only to be discharged 24 hours later due to the COVID pandemic.
For the next four years, we navigated our PFD journey the best we could. We transitioned to a new feeding therapist, continued to educate ourselves as best we could, adjusted medications and formulas, and continued to find ways to entice Jax to eat each day. It was exhausting not only for Jax, but for our entire family.
About six months ago, during a gastroenterology appointment, our doctor asked if we would be interested in trying the same outpatient program at the same hospital that had yielded limited results five years earlier. I was not expecting this. In fact, I had an evaluation scheduled in six weeks for the same inpatient feeding program we had been exited from during COVID. I realized we had a unique opportunity on our hands.
We had five years of growth, food exploration, development, and maturity on our side, while the hospital had five years of adjustments, learning, and experience on their side. I cancelled our inpatient feeding program evaluation and decided to give the outpatient program another try, but this time, I wanted to prepare myself for each step of the journey.
I reached out to friends, therapists, doctors, and various people at Feeding Matters to help us prepare for our program evaluation as well as our next steps. Their collective insight gave me a fortified view of how this experience could be different.
Follow the next chapter in Amber and Jax’s story by visiting our blog regularly. Updates to come!
A case for giving: Why gifts to Feeding Matters matter
Published by Feeding Matters on Nov 27, 2023
Feeding Matters is the only organization where education, advocacy and support for pediatric feeding disorder (PFD) is our passion and purpose. In this season of nonprofit giving, one supporter explains why her family chooses Feeding Matters for their charitable giving.
From the day Kirbi Lamb’s first son, Finn, was born, she knew something was wrong with feeding. “He was just totally not interested in eating, literally from the moment of birth,” she says.
She reached out for support from the hospital providers, but everyone told her it wasn’t unusual. On the day of discharge, Lamb finally met a lactation consultant who handed her a nipple shield and formula.
Lamb was sent home with a baby who refused to eat and never did manage to breastfeed. She pumped, but her baby only took a little bit from a bottle. Milk dribbled down the sides of his mouth, and he vomited nightly.
Lamb and her son were at the pediatrician’s office once or twice a week. There, she also felt like she wasn’t being heard. Her baby was still steadily growing, thanks to the Lamb family’s sheer determination to feed him. Everyone told her spitting up and vomiting was normal.
It took 10 months until they finally got a referral for a swallow study. They discovered he was aspirating so badly that his liquids had to be as thick as honey. “That was the day I broke when they told me my child had been aspirating all this time. I was holding it all together until that day,” she says.
 Since then, Finn, who’s now 7, has undergone feeding therapy, medical testing, laryngeal cleft surgery and an intensive feeding program. He never got an official diagnosis to explain the exact issues. What was clear is that from birth, it was hard to swallow, and gastrointestinal issues made eating more uncomfortable. Today, he eats about 20 different foods.
Since then, Finn, who’s now 7, has undergone feeding therapy, medical testing, laryngeal cleft surgery and an intensive feeding program. He never got an official diagnosis to explain the exact issues. What was clear is that from birth, it was hard to swallow, and gastrointestinal issues made eating more uncomfortable. Today, he eats about 20 different foods.
One of the most challenging parts of navigating their son’s feeding issues was not knowing what was wrong and not being believed. When Lamb’s second son was born with similar issues, the family knew how to help him from the start.
 Since becoming a parent of a child with PFD, Lamb has been dedicated to supporting the education and advocacy work of Feeding Matters. “It’s the only organization where pediatric feeding disorder is their passion and purpose,” she says.
Since becoming a parent of a child with PFD, Lamb has been dedicated to supporting the education and advocacy work of Feeding Matters. “It’s the only organization where pediatric feeding disorder is their passion and purpose,” she says.
PFD impacts 1 in 37 children, making it more prevalent than autism and cerebral palsy.
Still, even providers need the education Feeding Matters offers, says Lamb. “Providers still don’t know what they need to know about feeding disorders. Everyone thinks it’s picky eating.”
The Lamb family are generous donors to Feeding Matters. She says, “I want other people who are going through it to know what to look out for and that there are others out there going through this.”
How Feeding Matters uses charitable gifts to support families and raise awareness about Pediatric Feeding Disorder
Feeding Matters is a 501c3 nonprofit organization that operates on grants and charitable gifts from generous donors. We have the highest possible rating on Charity Navigator of 4 stars.
Charitable gifts to Feeding Matters are used in the following ways.
Family financial assistance program:
Raising a child with PFD is expensive. That’s why we offer grants to help support families in need. Grants are used for formulas, care and medical costs.
In 2023, 4 families were awarded $2,500 each.
Advocacy:
We advocate for policy changes and increased awareness of pediatric feeding disorder on a national and international level. We were the catalyst for the name and code for PFD, which is the foundation for all future system changes.
Research:
A lack of longitudinal, evidence-based data and the diverse nature of PFD are barriers to understanding the individualized needs of children with the disorder. Together with our PFD Alliance, we strive to identify, fund and facilitate research and clinical studies that address these issues. We aim to move the field from using practice-based evidence to relying on evidence-based practice.
Education:
We provide crucial resources and support to families navigating the challenges of PFD. We facilitate professional educational initiatives for clinicians, ensuring healthcare providers are equipped with evidence-based knowledge and tools. XX clinicians joined our International PFD Conference in April.
Whether you are a long-time supporter or are giving for the first time, thank you for helping us improve the lives of children with pediatric feeding disorder. We are grateful for donations of all sizes.
Donations made to us are generally tax-deductible in accordance with applicable laws. Click here to donate.