The Power of Trauma Informed Care for Children with Pediatric Feeding Disorders
Published by Feeding Matters on Apr 05, 2023
Of all the clinical appointments for 15-year-old Maya Roberto over the years, one stands out. Instead of catatonically going through the motions of her echocardiogram, Maya interacted with her cardiologist, even asking questions. Her mother, Dr. Anka Roberto, recalls how shocked she and her doctor were as Maya actively engaged with her cardiologist for the first time.
Noting that his patient, who was five years old at the time, was much more lively, the physician asked what had changed. Roberto, DNP, MPH, APRN, PMHNP-BC told him, she was in trauma therapy and just had an Eye Movement Desensitization and Reprocessing (EMDR) session to help her work through her medical trauma.
The doctor had never heard of it, and was pleasantly surprised with its efficacy.
Today, Roberto uses EMDR to help heal her pediatric patients from trauma as a private practice clinician.
Roberto’s years as a NICU nurse and mother of a child with complex congenital heart defects prepared her for a career in trauma-informed care as an advanced practice nurse. She’s seen personally and professionally how much treating a patient’s trauma as part of the continuum of care can make a difference.
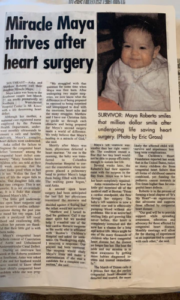
Since birth, Maya’s journey has included multiple open heart surgeries, years of feeding therapy and an NG tube. Roberto knows firsthand how traumatic medical and feeding interventions can have a lasting impact. For children with pediatric feeding disorder (PFD), considering and treating medical trauma can go a long way toward healing children.
Trauma-informed care offers a comprehensive approach that considers emotional and mental well-being to help children and their families affected by PFD. Understanding the impact of trauma on the body and how to navigate it allows families to access an effective care modality.
Defining trauma
Trauma varies for everyone. One major incident or many minor insults can cause trauma. Two people experiencing the same situation can respond entirely differently. One can move forward, while the other carries a lasting physical and emotional imprint. “When I think about trauma, it’s more of an adversity,” says Roberto. “We could have a big trauma, or we can have little things that add up to carry the same weight of a big trauma.”
What matters is how trauma affects the brain and body.
The CDC-Kaiser Permanente Adverse Childhood Experiences (ACE) study is one of the most comprehensive investigations into the lasting effects of childhood trauma. The longitudinal study showed that early adversity could significantly impact future physical, social and emotional health – as well as lead to early mortality rates.
The pandemic further raised awareness of how trauma can affect mental and physical health.
How the body reacts to trauma
Trauma can profoundly affect the body. Potentially traumatic experiences trigger the body’s “fight or flight” response. In this state, the heart rate increases, and respiration speeds up as the sympathetic nervous system prepares to defend against danger.
The disruption of hormones and enzymes caused by the experience can lead to difficulty regulating temperature, breathing and digestion. The gastric emptying system turns off. It causes constipation, loss of appetite, and/or motility (muscles in the wall of the gut) issues.
“It’s like the fire alarm in the house is going off,” says Roberto. When this happens, the parasympathetic system, sometimes called the “rest and digest” system, stops working.
These acute responses can make an imprint that has long-term effects. Families of children with PFD can mitigate the impact of trauma with support and care. “Trauma leaves a mark, but it’s up to us to find those who can help us get out of being stuck in the triggered cycle,” says Roberto
Understanding trauma-informed care for children with PFD
Trauma-informed care is an approach to support those who have had adverse experiences during their lifetime. Unlike traditional forms of care, which may not be sensitive to traumatic experiences, trauma-informed care recognizes the impact of trauma on an individual’s behavior, thoughts and emotions. The goal is to create a safe space for healing and recovery.Trauma-informed care involves four key components, known as the “Four R’s:
- Realizing how trauma can affect an individual
- Recognizing signs an individual has experienced trauma
- Responding effectively with appropriate interventions
- Resisting re-traumatization by promoting safety, trust, empowerment and collaboration
Understanding these components is essential to effectively support children with PFD, who may be dealing with the long-term effects of traumatic experiences.
Trauma can disrupt eating patterns by causing fear or anxiety around food, leading to refusal or avoidance behaviors. This compounds feeding issues children with PFD already experience.

For children with PFD, trauma-informed care offers a safe way to explore emotions while helping them build positive relationships around eating.
How to navigate the impact of feeding trauma
The effects of trauma on children with PFD can be challenging. What’s traumatic to one child may barely register for another. And the traumatic experience often isn’t even something the child can recall.
This is why it’s crucial to understand each child’s experience, recognize triggers and provide emotional support. Therapeutic interventions such as EMDR can help children reprocess past traumas without needing to talk about them. In her practice, Roberto uses a sand tray and play therapy to help children process previous experiences and feelings.
“They may not have verbal recall and a story to tell, but they remember feeling a certain way,” she says.
A child’s visit to a doctor’s office, for example, can trigger a panic attack because they don’t want to lie on the table, says Roberto. “It’s really because of this unprocessed adversity, which for many people may come from a place of not having control.”
With EMDR, she helps children uncouple the emotional tenacity from that memory.
Benefits of trauma-informed care for children with PFD
Trauma-informed care provides a safe space for families to build trust and better understand how to support their children. Trauma-informed care allows children to explore the experiences that triggered their trauma and develop improved emotional regulation skills. It can also lead to an improved appetite and a willingness to try new foods.
When children get emotional support, they can better articulate their needs to their parents and healthcare team. A therapist can help a child develop practical communication skills and problem-solving techniques. With practice and guidance, these tools allow children facing medical trauma to cope more effectively in difficult situations.
3 ways to support children with feeding trauma
Finding the right resources for trauma-informed care can be challenging, but more resources are developing with a heightened awareness of trauma’s impact.
Focus on the whole family
Roberto says supporting the entire family is key to helping children heal from traumatic events. “Families are like a tree, so if one limb is struggling, the others will start to wither as well.”
Give kids time
Children with medical complications react to stress in the same instinctual way as anyone who senses physical danger. Anyone who’s had to submit their child to medical testing has likely witnessed the fight, flight or freeze response. Roberto recommends slowing down in those moments. “Listen to your kids and give them the time to get there. It’s not about our agenda, as parents or as clinicians. It needs to be about the child’s agenda and providing them with the support they need in the moment.”
Get outside support
Talk to your child’s doctor or pediatrician about what type of care is available in your area and look for mental health providers who specialize in this trauma-informed therapy.
Online resources can also be helpful when seeking out trauma-informed care. The National Child Traumatic Stress Network offers comprehensive information geared toward helping families affected by traumatic events.
Finally, it’s important to remember that although trauma can be difficult, it can be an opportunity to move forward and break the trigger cycle. Roberto says, “We all have our experiences, but we don’t have to let them define us or limit our future possibilities.”
By understanding the trauma children with PFD can experience and working through it with compassion, children can regain control over their lives and reach their full potential.
Anka Roberto, DNP, MPH, APRN, PMHNP-BC an assistant professor at the University of North Carolina Wilmington and has authored book chapters and numerous publications on trauma and resilience. In her private practice, Holistic Healing, PLLC, she provides functional psychiatry care and EMDR therapy to target and reprocess negative life experiences across the lifespan.
Roberto is the keynote speaker at the 10th Annual International PFD Conference on April 13-14. Click here to learn more and register.