Insider insights: Preparing for your child’s G-tube journey
Published by Feeding Matters on Feb 26, 2024
What to expect before and after your child’s G-tube insertion
So, you’ve finally decided to get a G-tube for your child. Arriving at this point in your child’s feeding journey can be a relief. Others may feel some regret.
Either way, says Karen Ellis, mother of a 2.5-year-old who recently got a G-tube, getting a G-tube can make life a lot easier for children with pediatric feeding disorder (PFD) and their parents. After a minor procedure, a short recovery and months of stress-free feedings, Ellis and her family are confident they made the right decision for their son.
G-tube insertion, or gastrostomy tube insertion, is a medical procedure where a tube is placed through the abdominal wall and into the stomach. This allows caregivers to deliver nutrition and medications directly into a child’s stomach. Some kids with a G-tube use it to supplement oral feeding. Others exclusively eat and drink through the device.
Learn more about the benefits for kids with PFD of G-tubes in this blog: Does your child need a G-tube? Here’s what you need to know.
Ellis’s son, Ishan, gets most of his nutrition through the G-tube. He eats and drinks orally as well. Ellis offers insight into what parents can expect from the G-tube procedure and the few months after it.
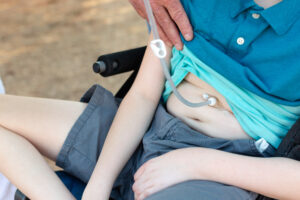
What to expect before the G-tube procedure
Ishan had an NG tube for a longer period than typical, says Ellis. Running after an active toddler to replace the tube whenever it fell out was a constant struggle. Since birth, Ishan has struggled with eating due to gastrointestinal issues and silently aspirating. He was often sick, didn’t eat age-appropriate amounts and was slow to gain weight. His parents pushed Ishan’s providers to consider a G-tube, but they were told their son might grow out of his feeding issues.
At this stage of the PFD journey, Ellis says following your instinct as a parent is essential to advocating for your child’s needs. “They wanted to blow everything off as normal parenting or a simple therapy issue, but knowing as a parent that there continues to be something wrong means you have to keep pushing,” she says.
What gave Ellis clarity, she says, was knowing they were trying hard enough. “He was doing his best, we were doing our best, but still, something was not quite right.”
What to expect during the G-tube procedure and recovery
For Ellis, the hardest part of the G-tube procedure was knowing it was elective surgery that required hospitalization. By the time Ishan was scheduled for surgery, Ellis knew it was necessary, but she still felt they had made a choice. Ishan’s procedure and recovery both went smoothly.
Like most kids, Ishan spent one night in the hospital. Ellis says he did experience some pain that first and second day. Ishan received pain medication and lots of TLC. They held him the whole time at the hospital and watched his favorite programs.
By day three and four, Ishan was back to running around and doing his typical gymnastics flips. He returned to his normal toddler antics in less than a week. “Kids are resilient, but we tried to hold him back from too much activity right after surgery,” she says.
For two weeks, Ishan had to skip his baths and only have sponge baths. In general, swimming in the pool or ocean tends to be okay, but lakes and rivers can be problematic.
Watch the skin around the G-tube because that can start to look angry and red initially. You can learn more about feeding tube care using What You Need to Know Now: A Parent’s Introduction to Tube Feeding. This resource, also provided in Spanish, was provided by the Feeding Tube Awareness Foundation with permissions to share.
What to expect in the months after a G-tube procedure

Adjusting to G-tube feedings takes some trial and error for parents and kids. Even months later, G-tube feeding requires adjustments when a child is less hungry due to an illness or more hungry due to a growth spurt. In the beginning, says Ellis, it’s important to go low and go slow with feeds.
At first, Ishan hesitated to let anyone touch his stomach, so his parents made buttons for his favorite stuffed animals. They fashioned these themselves, but you can also buy them. Ellis showed Ishan how opening and closing the button doesn’t hurt. They spent a lot of time talking about the button and getting used to it before diving into feeding.
Ellis also spent some time getting used to feeding her son through the tube. Overfeeding can cause vomiting or an upset stomach. She keeps a towel in the car in case of any incidents. “It’s hard to guess how much a toddler wants to eat. It’s never a perfect science,” she says.
Ellis offers three tips for G-tube feeding
- Find the formula your child tolerates best. Like baby formula, G-tube formulas come with different ingredients. The Ellis family found that the vegan formula has been better for Ishan than the milk formula.
- Stay consistent with oral feeding when applicable. Ishan eats orally two times a day. They do this before tube feeding so that his stomach isn’t full.
- Use a backpack. Cute feeding backpacks allow busy toddlers to run around independently during feeding sessions. Ellis tapes the tubing to the back of Ishan’s shirt or pants so it doesn’t come out while he’s running around.
These days, Ishan is happily playing and growing, and his parents are confident they made the right decision to get a G-tube. Ellis says it’s helpful to consider the G-tube feeding experience with PFD more like a marathon than a sprint. This can be harder for parents than kids, who tend to be more resilient. “As long as the kid is pretty happy and healthy, we’re the ones who are more stressed,” she says.
For more support in your G-tube or pediatric feeding disorder journey, check out our peer-to-peer mentoring program.